Among all fungal diseases, mycoses (fungal lesions) of the skin of the feet are the most common. They are also called ringworm or athlete's foot. Approximately 30% of the population have problems with diseases of a fungal nature. Almost half of the patients never go to the doctor with them, spreading the fungus among their loved ones. Microscopic pathogens affect the dermis (skin) or nails. In the latter case, they speak of onychomycosis.
Why are the feet the most affected?
Various fungi are always present on the skin. Their reproduction is restricted by beneficial bacteria and skin secrets. In case of violations in the work of immunity, changes in the composition of the skin microflora, a favorable moment arises for fungi - they can multiply freely. Entry gates for infection can serve as regular damage:
- scratches;
- cracks;
- excoriation.
Another cause of mycoses is endocrine disorders. In case of a malfunction in the work of the endocrine glands, not only the balance of hormones changes, but also the work of the whole organism. Even the composition of the secrets of the skin changes, due to which they lose their bactericidal properties. Fungi can feed on them, which also favors reproduction.
Other factors also contribute to the weakening of protective forces:
- food depletion (malnutrition);
- avitaminosis;
- excessive physical and psycho-emotional stress;
- concussions;
- usual stress.
All of these are non-specific causes of fungal skin lesions. Due to them, mycoses of the feet, smooth skin on the body or mucous membranes can develop.
In addition, there are special types of fungi (genus Trichophyton or Microsporum) - pathogens (pathogens). In contact with the skin or on its surface, they cause diseases. In the case of the feet, the disease is called rubromycosis. On the body, these pathogens form specific spots - lichens. You can get infected from a person or an animal.
The skin of the feet is a special place for fungus. There are always many keratinized cells. Microbes are used as housing and food. "Rampant" fungus contributes to sweating of the feet. In closed shoes, a moist, nutrient-rich environment is formed on the feet - the "dream" of each fungus. If a person neglects foot hygiene, does not dry and disinfect shoes, the infection first multiplies, and then passes to the feet of the "owner". Poor hygiene products, dry, synthetic socks also contribute to the spread of a fungal infection.
Signs of a fungus, visually perceptible.
Treatment of dermatomycosis is easier the sooner the disease is diagnosed. In advanced cases, therapy is long term, involves taking pills and using external agents. In the initial stages of mycosis you can do without ointments. It is important to be able to recognize the first symptoms of the fungus in order to see a doctor in time.
The appearance of the fungus depends on the form of the mycosis. Fungal infection of the feet can occur in 3 different variations, as well as in a mixed form, when the signs of all three main varieties are present on the legs at the same time.
intertriginous form
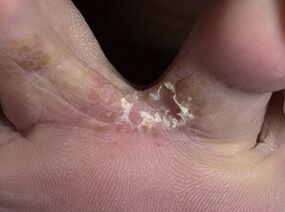
A type of tinea pedis that mainly affects the skin between the toes. The first symptom of the disease is the appearance of a painful crack between the 3rd and 4th or 4th and 5th hoops of the foot. The damage is small, but it causes discomfort when washing your feet and walking.
If you carefully examine the wound, a whitish stripe is noticeable around it (example in the photo). This is what the edges of the skin look like around the peeled crack. The wound can itch, fester, increase, or vice versa - periodically heal, and then reappear.
In some cases, the fissure heals, but the skin continues to peel off, hyperkeratosis (thickening of the dermis) develops, calluses and corns appear. With the advanced intertriginous form, the cracks are enlarged (example in the photo), they appear between other fingers, the skin is constantly moistened. It is difficult for the patient to move, wear shoes.
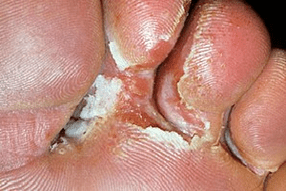
As you progress in this form, the rift increases in size. Similar signs appear on the second foot. Thick, large layers of skin exfoliate around the wound. The second (attached) end is not pushed back, and attempts to remove the keratinized part with fingers end in additional damage to the foot.
This type of foot fungus is the most common. The manifestation of the pathology at first is not accompanied by any symptoms. As a rule, the infection develops between the 3rd and 4th fingers and does not change the color and structure of the skin to a certain extent. After that, wet cracks and layers of skin appear.
The foot itself remains unharmed, however if the fungus is affected the feet may sweat more than normal. Therapy of the fungus of the intertriginous form is characterized by medium complexity.
dyshidrotic form
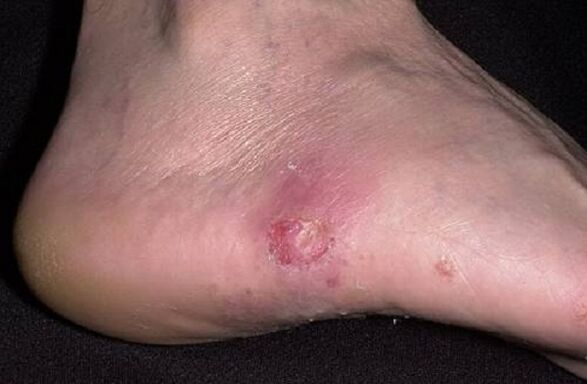
With this form, the first signs of a skin fungus are bubbles on the arch of the foot. Most often near the heel. The surface dries up, deep seals appear (they feel like nodules). Later, they noticeably rise above the plane of the skin, as they are filled with fluid. The vesicles (vesicles) are usually small, 2–5 mm in diameter. They can merge, forming larger ones - blisters. Other symptoms include pain and itching around the rash.
The progress of the dyshidrotic form of mycosis is manifested by the bursting of blisters. In their place, small or large erosions are formed. Often they become infected with bacteria and begin to boil. Erosions do not heal for a long time, which makes walking painful. In some cases, the erosion disappears and dryness appears in its place.
scaly shape
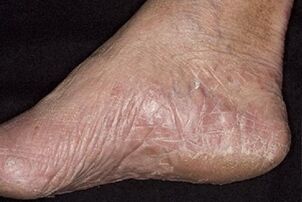
With the progression of the disease, severe hyperkeratosis of the feet develops. The size and number of cracks increases. The biggest ones can bleed. Such damage is the pathway for the invasion of other pathogenic microbes into the body. Therefore, wounds periodically become inflamed, can abscesses. The most common form of foot fungus is manifested by increased dryness of the skin on the plantar part of the limb. It can mean a recent accession of the fungus, or vice versa, be the result of the development of other forms.
On the arch of the foot and in the center, the dermis becomes dry, thin, shiny, covered with a mesh of grooves. In the area of the fingers and heels, hyperkeratosis is observed - rapid keratinization, in which dead particles do not have time to exfoliate. Calluses or calluses form on the forefoot. There are small cracks on the heels. The entire surface is rough due to pronounced peeling. The patient may experience itching. With the prolonged development of mycoses, this symptom is absent.
You can determine the fungus on the legs by excessive dryness, unpleasant odor, itching and constant peeling of the skin.
onychomycosis
Onychomycosis is a type of fungus of the foot (or palms), which affects the appendages of the skin - the nails. Nail fungus can be caused by the same pathogens that cause mycoses on the skin. Catching mold and other types of monofungi in the nail salon, at the beach, trying on new shoes in bare feet, going to the sauna or swimming pool. An ingrown toenail can be a contributing factor. The thumb is most commonly affected.
When it hits the nail plate, the fungus begins to divide. It penetrates deep into the nail, spreads over its area. The first signs by which you can determine the fungus on the nails are loss of shine, the appearance of spots (white, yellow, brown, greenish), a change in the shape of the nail plate.
As the disease progresses, the structure of the nail changes in the zone of discoloration (it thickens, becomes irregular, loose).
Running toenail fungus looks like thick, yellow growths. It is difficult to care for affected nail plates. Before each trimming, you have to make hot foot baths. After contact with water, the nails become smoother and easier to remove with manicure tools.
If the nail fungus is not treated, onycholysis begins - the plate is completely or partially exfoliated. After removing its remains, the nail does not always grow back. Sometimes the detachment process ends with the complete loss of the nails.
General principles of treatment

The fungus on the feet is treated with special ointments, creams, solutions, varnishes. In parallel, the patient is prescribed antifungal tablets.
During the entire duration of treatment, careful hygiene of the feet is shown, weekly cutting and sawing of the damaged part. Every day, the patient must remove the layer of keratinized cells from the surface of the feet, using a pedicure file.
It is also important to carefully care for shoes - treat them with antifungal drugs or disinfectants. The shoes are dried and aired daily in the open air.
external media
Ointment or cream is prescribed only in the initial stages of foot fungus. For treatment, a cream and other medications are prescribed. They are applied to the skin 1-2 times a day, after washing the feet well with a simple soap. Before using creams, it is important to completely dry the feet. Do not apply the medicine to wet skin. After the treatment, the patient should wear cotton socks.
tablets
It is impossible to treat the fungus with pills on your own. All drugs negatively affect the functioning of the liver and kidneys, have a number of contraindications. Before prescribing a course of antifungal tablets, the specialist will recommend taking a general and biochemical blood test, which can be used to assess the condition of vital organs.
nail preparations
Useful in the treatment of onychomycosis and foot fungus. In the first case, they are used to remove the affected part of the nail, in the second - to prevent infection of the nail plates with fungi.
It is more convenient to be treated with varnishes - they are applied to the nails 1-2 times a week. The most affordable drugs for nail fungus are solutions, they are applied to the nails 2 times a day until complete recovery. Special gels are popular. They visually improve the condition of the affected nails, along the way, they stop the reproduction of the fungus. Ointments are also prescribed for onychomycosis. They are applied in a thick layer on the affected plaques, covered with a bandage, kept like this until the product is completely absorbed. The treatment is repeated twice a day.
Preventing foot fungus is much easier than treating it. To do this, you need to lead a healthy lifestyle, take your own slippers to the pool and sauna, regularly wash and air your shoes, wear socks made of natural fabric, and use antiperspirant products. With regular visits to "wet" establishments, you need to use antifungal creams prophylactically - treat the skin of the feet 1-2 times a week.
















