A third of people in the world have stratification and crumbling of the nails, darkening of the plate.
This disease is called onychomycosis or nail fungus. It can start at any age, spreads instantly, and adapts well to different conditions.
%20and%20those%20affected%20by%20fungus%20(right).jpg)
Reasons for the formation of onychomycosis
Infection with a fungus is quite easy. The infection can be found inpublic showers, beaches and swimming pools.There is a high risk of contracting onychomycosis from infected loved ones and relatives if household items are used together.
There are the following prerequisites that provoke the entry of the pathogen into the body, in short, the causes of the appearance of the fungus:
- small lesions on the skin of the feet (corns, calluses, small cracks and abrasions) that are produced by tight footwear;
- weak immunity due to inflammatory and infectious diseases;
- vascular ailments, impaired functioning of internal organs, which leads to difficulties with blood circulation in the legs;
- violated safety precautions, that is, going to public places without shoes, poor foot hygiene, trying on someone else's shoes;
- ignoring profuse sweating and diaper rash on legs.
Important!
Onychomycosis starts on the thumb and the virus can later develop on the little finger.
What diseases can serve as a prerequisite?
The risk group includes people whose skin does not breathe due to tight shoes throughout the day. These include representatives of working specialties.
There are the following diseases that can serve as a prerequisite:
- diabetes mellitus groups I and II;
- phlebeurysma;
- foot deformity;
- obstruction and blockage of blood vessels.
Today, various creams and varnishes are often offered for treatment, however, they will be useless, since the cause may be caused by internal ailments.
types of infection
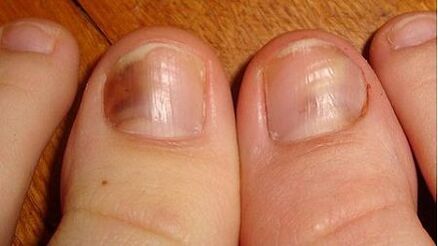
In total there are more than half a thousand species of fungi.bringing trouble. There is no single classification.
The only thing is that there are two important signs by which the disease is distinguished. This is the localization and type of pathogen.
Important!
The infection can be anywhere on the nail, and this is the main symptom of the disease. Externally, the affected plaque changes depending on the localization of the virus.
Pathogen type
There are different causative agents of the disease, each of which has its own distinctive characteristics. These are important to consider when developing a treatment plan. The most common pathogens are:
- dermatophytes- this is trichophyton red and mentagrophytes, epidermophyton scaly, etc. When infected with such fungi, yellowish or grayish spots are formed, the remaining parts of the plaque become cloudy, and the free edge changes in shade. In general, the entire surface changes and eventually moves away from the bed.
- molds. This type is relatively harmless. It does not penetrate into the deep layers of the nails, therefore it only changes the plates to a dark, swampy, gray, yellowish, brownish color. Such a shadow can affect the surface both partially and completely.
- Yeasts of the genus Candida. They thin the nail and contribute to its exfoliation. Often, due to this pathogen, a white form of the disease is formed, which is characterized by inflammation of the cuticle. They can cause severe pain, and purulent discharge may be observed. If left untreated, the nail will thin, turn brown, and pull away from the bed entirely.
Places of localization of the disease on the arms, legs.
The main forms of onychomycosis:
- Side.There is a nail infection on the sides. Its color becomes gray, yellowish and brownish. The dish begins to cloud, crumble and exfoliate.
- Distal.This is the most common type of fungus. The infection starts from the free edge of the nail. The plaque changes color to yellow, brown, or gray. As time goes by, the loss gets bigger. Delamination, crumbling and clouding begin on the plate. In this case, hyperkeratosis appears under the nails, and if the entire nail is affected, tissue dystrophy is formed.
- proximal.This form implies damage to the cuticle, which swells, becomes inflamed, blushes and changes its shape and structure. As a result, the roller separates from the plate, and the nail crumbles, fades and is deformed. With a neglected disease, the plate can completely fall apart.
- white surface.It appears, as a rule, on the thumb, on others - occasionally. Outwardly, it manifests itself in the form of white spots that are located over the entire surface of the nail. Further, the disease progresses and spreads to keratinized tissues. The spots may change color, from milky to green or yellow. The plate structure becomes spongy and loose. If this form is not treated, the nail can completely collapse.
- The dystrophy is total.Covers the entire surface of the nail. This is an advanced degree of distal or proximal fungus. The plaque thickens, changes its shape to an unnatural shape, and eventually completely deteriorates.
Photo of mycosis on the nails
%20and%20with%20manifestations%20of%20onychomycosis%20(right).jpg)
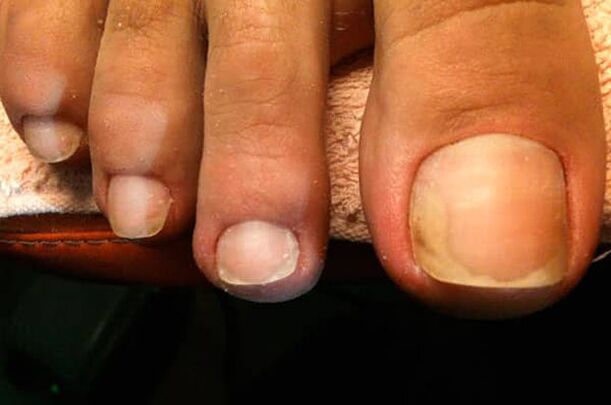
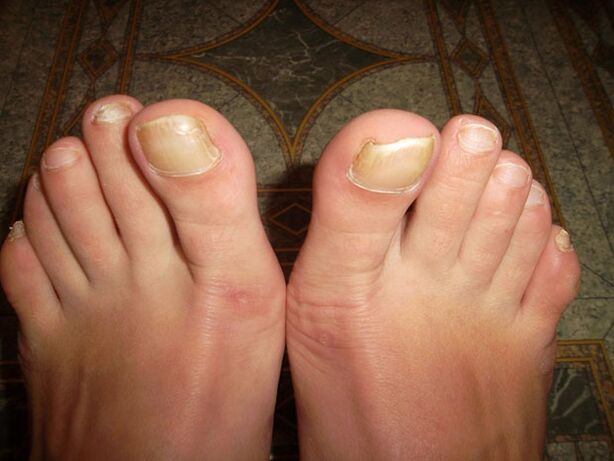
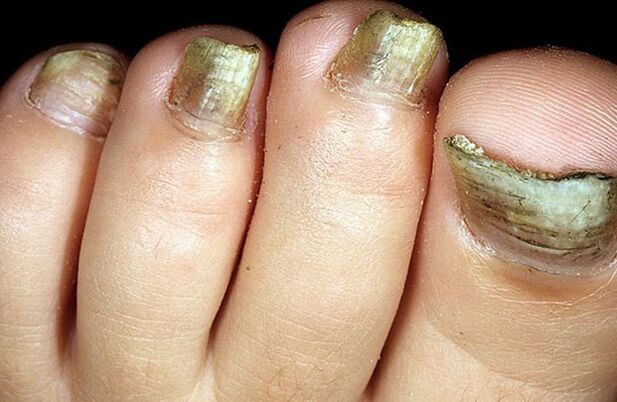
symptoms of mycosis
After an infection has occurred, the fungus needs time to take hold. First, the disease affects the big toes and destroys the nail plate. Damage is manifested by such signs as:
- Thickening.The plaque becomes thicker due to strong keratinization. In advanced cases, this significantly complicates treatment.
- Change of tonality.In a healthy state, the nail is translucent, and the translucent capillaries give a pink color. And the infected change their hue to black, brown and yellow. A space forms under the plate in which microbes and other pathogens develop.
- falling apartWith incomplete treatment or its absence, the fungus begins to penetrate into the deeper layers of the plate. As a result, it falls apart and collapses. If you do not carry out therapy, onychomycosis becomes chronic. Because of this, the immune system weakens, allergies begin, and problems with internal organs begin.
How to independently determine, recognize the disease?
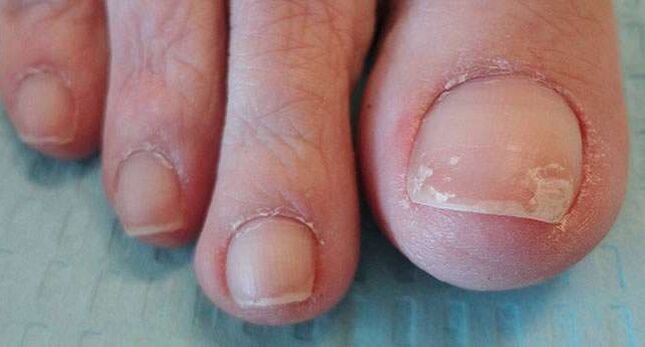
The fungus first affects one leg, then the infection moves to the second. It is not necessary to delay with this disease, if you yourself doubt and cannot determine the virus, be sure to consult a doctor.
You can diagnose it yourself at home using certain methods.
Find out with potassium permanganate
There is an express method that consists of immersing the feet in a potassium permanganate solution. At the same time, potassium permanganate stains healthy nails brown, and infected ones remain light.
This procedure is simple and does not require much time. A little potassium permanganate is added to a container of warm water. The solution should not be strong. Feet or hands are placed in the liquid and waited for about 10 minutes. This method is completely harmless. It can not be used alone if there are allergic reactions to potassium permanganate.
detect with iodine
Iodine is also often used to identify nail fungus. But it does not indicate the presence of pathogens. It can help eliminate other fungi, such as tinea versicolor.
When redness and peeling appear on the skin near the nail, they are treated with iodine. Healthy skin does not darken with an alcohol solution, and the area affected by lichen becomes very dark.
How to diagnose?
Today, several effective diagnostic methods are offered, probably the most reliable way is testing for nail fungus:
- Microbiological diagnosis.Microscopy is the most widely used method to detect fungi and determine their type. It allows you to detect infections only in the structure of the nail plate or skin tissues. Taking a biomaterial involves scraping infected cells from the area where the pathogen is found.
In the final and middle stages, fungal spores, yeast cells, and mycelium strands are found in the specimens. Such diagnosis makes it possible to establish the accumulation and type of pathogen. The procedure itself lasts from 2 days to a month.
- Linked immunosorbent assay. Such an analysis is designed to identify fungi that have affected both the nail and internal organs. Its difference is that to detect the disease, venous blood is required, which is taken in the morning or 4 hours after eating. No special preparation for analysis is required.
- PCR test.Polymerase chain reaction is the best diagnostic method for infectious diseases. It has a number of advantages, including speed, higher precision, and the ability to take any tissue sample. A narrow focus is considered to be a feature of the method. That is, for the diagnosis of onychomycosis, it is necessary to know exactly the place of localization. A PCR test can reveal both the type of fungus and its concentration in the body.
- luminescent study. Such a diagnosis is based on transillumination of the skin affected by pathological microflora with an ultraviolet lamp. When examining a patient, a Wood's lamp is used, which emits ultraviolet rays. Thanks to her, the products of vital activity begin to shine brightly. The type of pathogen affects the shade of the gloss.
How to distinguish mycosis from bruises and other diseases?
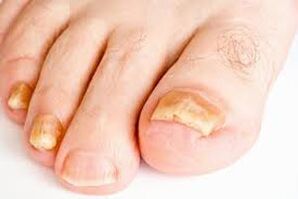
At first, onychomycosis is easily confused with other diseases, such as lichen, nail bruises, or psoriasis.
It can be distinguished by the darkening of the nail plate, the formation of yellow spots and stripes that enlarge over time and go deep into the nail.
Compared to psoriasis, onychomycosis runs smoothly. Little by little it deforms the plate so that it detaches from the bed. It is distinguished from lesions, psoriasis, lichens and eczema, the presence of pain and bad smell.
hygiene rules
The best remedy for fungus is prevention.Simple precautions can help prevent infection. First of all, they are needed by people who visit beaches, public pools, saunas, etc. In such places you should always use individual towels and use light slates.
If your feet sweat a lot, then you need to treat them with special means, of which there are many today. It is not recommended to wear shoes that are too tight or wear someone else's. When trying on shoes in the store, you should wear shoe covers or socks. Be sure to monitor the hygiene of the feet and hands, and dry them after washing.
When one of the family members is infected with the fungus, you should have a separate washcloth and towel. After visiting the bath, it must be treated with antimicrobial agents. The patient's wipe should be regularly treated with a 5% chloramine solution, and clothes and towels should be boiled with washing powder.
If there is a suspicion of infection, then the legs or arms should be immersed in hot water and held for about 10 minutes. The fungus dies quite quickly at a temperature of +50 ° C. Then these places are smeared with antifungal ointment.
conclusion
Onychomycosis is an insidious and unpleasant disease, so it is important to monitor your fingernails and toenails and make sure to follow preventative measures. If there are suspicious symptoms, it is best to see a doctor as soon as possible and start treatment.
















